|
Drugs like naproxen and ibuprofen may relieve pain and help reduce inflammation. Non-steroidal anti-inflammatory drugs (NSAIDs). Inflammatory arthritis can often be well controlled using medications, and it can go into remission when treated early in the course of the disease. Advances in the treatment of inflammatory arthritis have made a dramatic difference in the lives of people with these diseases. The treatment plan for managing your symptoms will depend upon your inflammatory disease. Inflammatory arthritis is often treated by a team of healthcare professionals, including rheumatologists, physical and occupational therapists, social workers, rehabilitation specialists, and orthopaedic surgeons. X-rays of an arthritic hip will show whether there is any thinning or erosion in the bones, any loss of joint space, or any excess fluid in the joint.Īlthough there is no cure for inflammatory arthritis, there are a number of treatment options that can help prevent joint destruction. 
X-rays are imaging tests that create detailed pictures of dense structures, like bone. 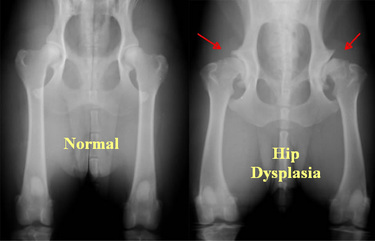
The doctor will also look for a limp or other problems with your gait (the way you walk) due to stiffness of the hip. Increased pain and limitation during some movements may be a sign of inflammatory arthritis. Physical Examinationĭuring the physical examination, your doctor will evaluate the range of motion in your hip. Patients with long-standing inflammatory arthritis or those who do not respond to medical treatment will end up with joint destruction, which can lead to joint replacement.ĭuring your initial examination, your doctor will ask questions about your medical history and your symptoms, then conduct a physical examination and order diagnostic tests. This is a physician that specializes in patients with autoimmune diseases. Patients with suspected inflammatory hip arthritis should be seen by a rheumatologist. Early diagnosis and treatment can help patients maintain mobility and function by preventing severe damage to the joint. Lyme arthritis (caused by Lyme disease)Īlthough there is no cure for inflammatory arthritis, there have been many advances in treatment, particularly in the development of new medications.Septic arthritis (caused by a viral or bacterial infection).Pseudogout (CPPD - calcium pyrophosphate dehydrate deposition disease).These diseases can also cause symptoms in the hip joint: There are also types of inflammatory arthritis that are not autoimmune in nature. Arthritis induced by immune checkpoint inhibitors (chemotherapy).Inflammatory bowel disease-related arthritis.Less common types of inflammatory arthritis affecting the hip joint include: These are common types of inflammatory arthritis that can cause symptoms in the hip joint: These diseases mostly affect the joints but can also affect other organs, such as the eyes, lungs, heart, gastrointestinal (GI) tract, and skin. Unlike osteoarthritis, inflammatory arthritis affects people of all ages, often showing signs in early adulthood. These types of arthritis are also known as autoimmune disorders. Inflammatory arthritis refers to any type of arthritis caused by an overactive immune system. OA typically causes painful symptoms in middle-aged people. Also known as degenerative arthritis, OA is associated with aging-related wear and tear or trauma it is not a result of the body's altered immune response. The most common type is osteoarthritis (OA), a non-inflammatory arthritis. 
The absence of normal hip passive adduction (LR− = 0.25 0.11 to 0.54) or abduction (LR− = 0.26 0.09 to 0.77) was useful in excluding OA.There are many kinds of arthritis that can affect the hip joint and make it difficult to do everyday activities. Physical findings associated with OA included posterior hip pain caused by squatting (LR+ = 6.1 1.3 to 29), groin pain on hip abduction or adduction (LR+ = 5.7 1.6 to 20), abductor weakness (LR+ = 4.5 2.4 to 8.4), decreased hip adduction (LR+ = 4.2 3.0 to 6.0), and decreased internal rotation (LR+ = 3.2 1.7 to 6.0). Findings associated with the absence of OA included being younger than 60 (negative likelihood ratio = 0.11 0.01 to 0.78), morning stiffness lasting less than 60 minutes (LR− range, 0.22 to 0.65), the absence of pain on walking (LR− range, 0.25 to 0.58), and the absence of pain improved by sitting (LR− = 0.24 0.06 to 0.92). Clinical findings associated with the presence of hip OA included a family history of OA (positive likelihood ratio = 2.1 1.2 to 3.6), a personal history of knee OA (LR+ = 2.1 1.1 to 3.8), pain when climbing stairs or walking down slopes (LR+ = 2.1 1.6 to 2.8), and the worst pain located in the medial thigh (LR+ = 7.8 1.7 to 37).
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
